Whenever your thoughts shift to end-of-life care and planning, you should consider having a DNR form. Patients have a right to decide what happens to their life after an illness or when they become elderly. This may involve obtaining a do not resuscitate form, which instructs medical professionals that you as a patient don’t wish to receive certain medical procedures such as CPR anytime your heart stops beating or you stop breathing. A DNR form is a very important legal document that patients in the situations mentioned above should have.
But what does a DNR form cover, how does it work, who needs it, and how do you go about it? This article will cover all the questions that you might be having about Do Not Resuscitate Forms.
What is the Do Not Resuscitate Form?
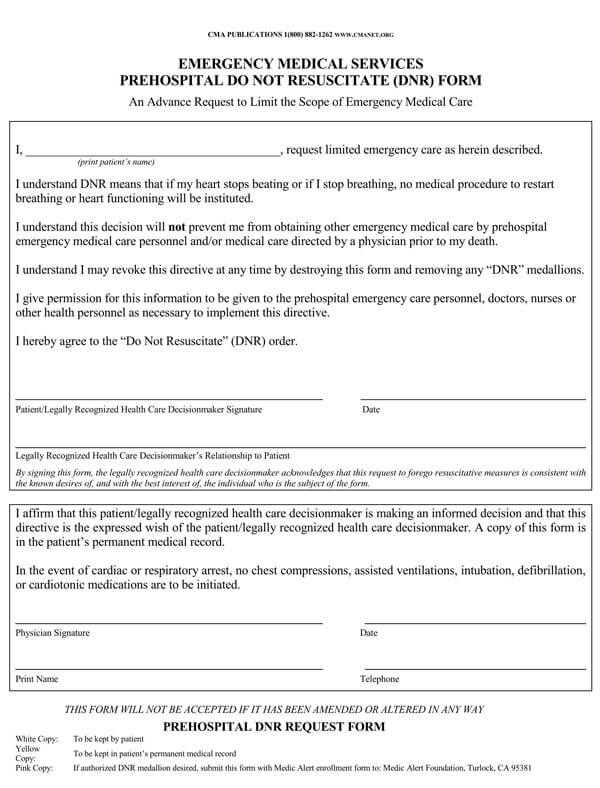
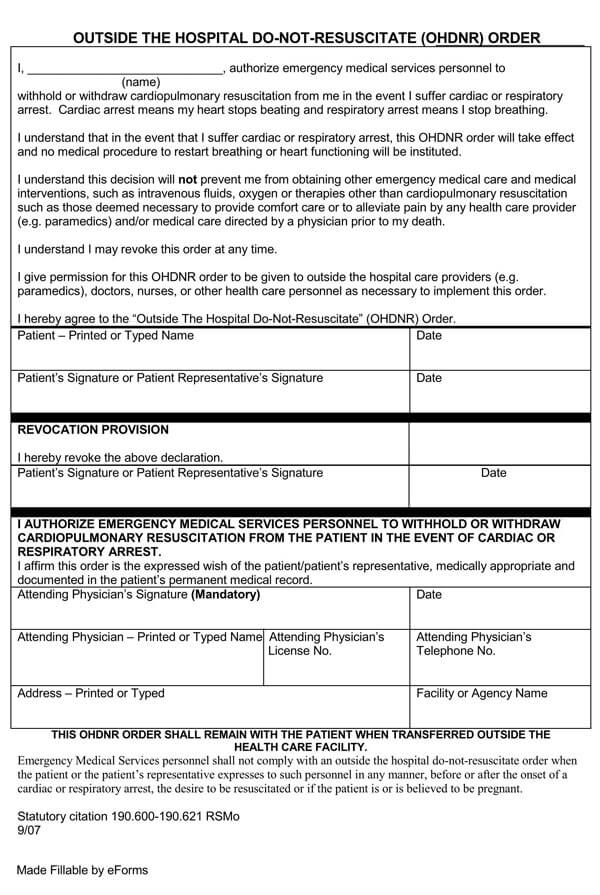
Do Not Resuscitate form, commonly abbreviated as “DNR Form” is a legal document that instructs medical workers not to use Cardiopulmonary Resuscitation (CPR), electric shock to the heart, artificial life support devices, or any other invasive procedures to resuscitate you once your heart stops beating or you stop breathing.
Healthcare providers are generally trained to do their best to revive a patient who has had a cardiac arrest or respiratory arrest. Without a DNR form, they will not honor your wish of allowing natural death. Cardiopulmonary Resuscitation procedures are not always successful, and they come with many risks, especially for elderly or terminally ill individuals. These procedures are only recommended for healthy patients.
Alternatively, a DNR form is known as a
- Do-not-attempt-resuscitation (DNAR) Order
- Allow-Natural-Death (AND) Order
- No-Code Order
Importance
Having DNR forms is part of advance care planning, essential for competent people of all ages. Obtaining a DNR means that your wishes for medical care are respected and adhered to, even if you lose the ability to advocate for them yourself. If an individual is incapacitated, health care professionals and emergency responders are obliged to pursue all potentially life-sustaining treatments to resuscitate your life in the event of a medical crisis unless a valid order is written by a physician such as DNR is presented.
With a DNR, one is able to participate in their own care decisions. This is because the document allows the patient some control over their care, even during emergencies. This saves your family and loved ones the difficult task of deciding on your behalf. DNR orders also prepare your family and loved ones to easily accept what happens to you in case of an emergency because they feel like they would be granting you your wish. This way, they’d be more likely to forget quickly and move on.
How do DNR Forms Work?
DNR forms may be included in a person’s living will or advance directive. All these documents allow you to express your preferences regarding end-of-life care if you are significantly incapacitated to communicate your wishes when the time comes. In any case, it is important to schedule a meeting with the patient’s doctor and thoroughly discuss all the possible aspects of implementing or deciding against a DNR form.
Once a patient successfully obtains a DNR order, it is then placed in the hospital chart- if you are admitted to a hospital. In this situation, you should keep your DNR form in a visible place so that first responders are likely to see it; otherwise, they will not know not to attempt resuscitation. It is also important that your family caregivers and loved ones are present in the hospital settings to advocate for your wishes if you are unable to advocate for yourself.
Nevertheless, suppose you are terminally ill, and you are receiving hospice care- which mainly focuses on symptom management rather than curative treatment. In that case, you should not worry about having family members advocate for you, as the hospice staff fully respects DNR orders.
It is important that you understand that DNR orders only affect the decision to receive CPR. All other essential treatments, such as palliative care, should be continued unless the patient or their loved ones says otherwise. For this reason, it is worthwhile that you consult your doctor to decide how a DNR order may affect other routine and life-sustaining procedures to ensure that everyone is on the same page.
Patients suffering from a terminal illness or at high risk of stroke, heart attack or respiratory arrest, or the elderly should consider having a do not resuscitate form. Nonetheless, even people with perfect health should consider acquiring this legal document, provided you feel strongly about not being intubated or resuscitated anytime breathing, or heartbeat has stopped.
What is an Advance Directive?
Just like a DNR form, an Advance Directive is a legal document that tells your doctor and family members what kind of medical care you would prefer to have if you are incapacitated and can’t inform them yourself. This may apply when a patient: is in a comma, is severely injured, is terminally ill, or is having severe dementia.
Physicians and healthcare providers tend to talk about advance directives to patients anytime they are admitted to a hospital. An effective Advance Directive should describe the type of treatment and care you would want if you have an illness that you are not likely to recover from. It should also describe the kind of care you would want if you are in a situation where you are permanently unconscious. The same should also be clear and inform your doctor that you don’t wish to receive certain kinds of treatment. Additionally, it should inform your medical personnel to give you a certain treatment no matter how ill they think you are.
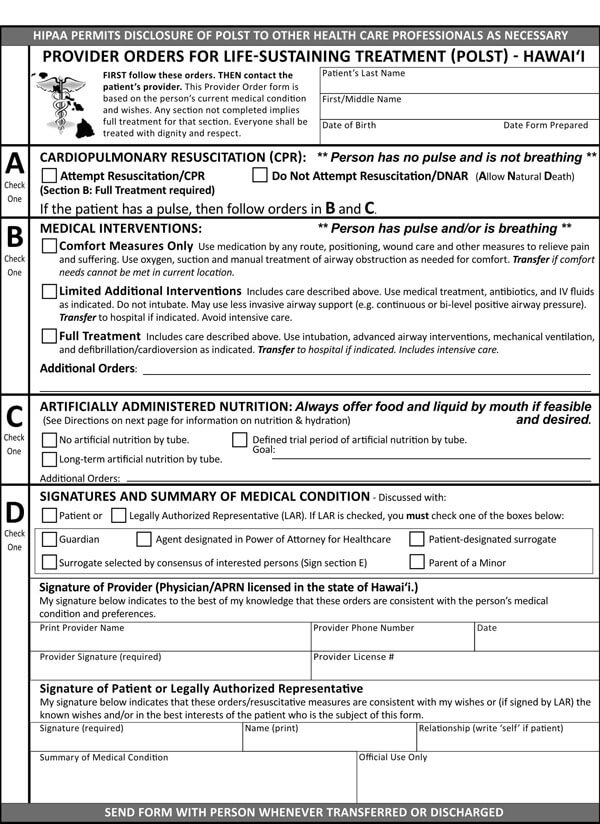
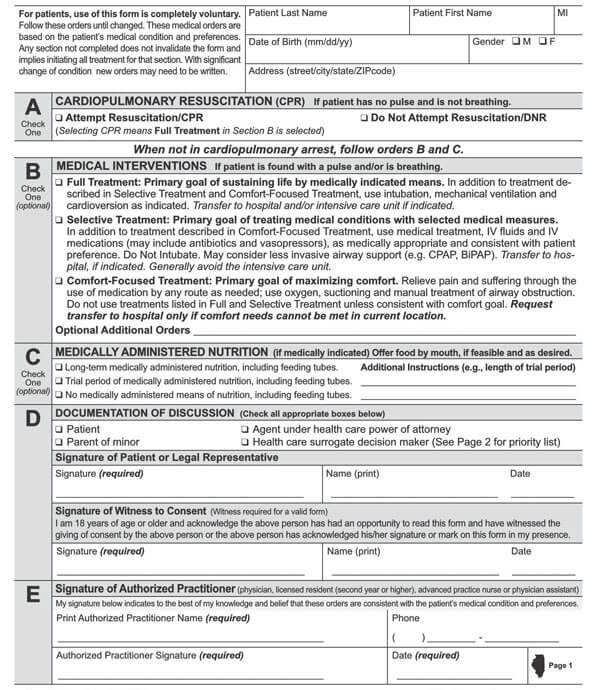
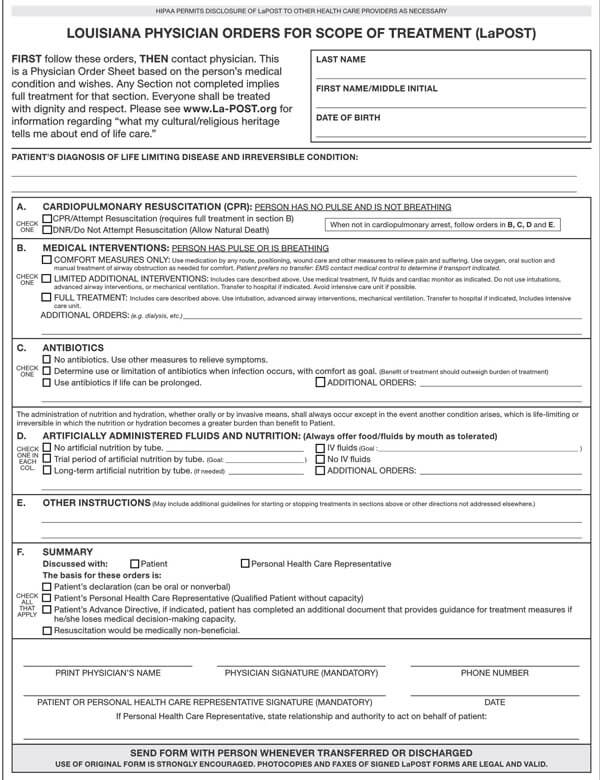
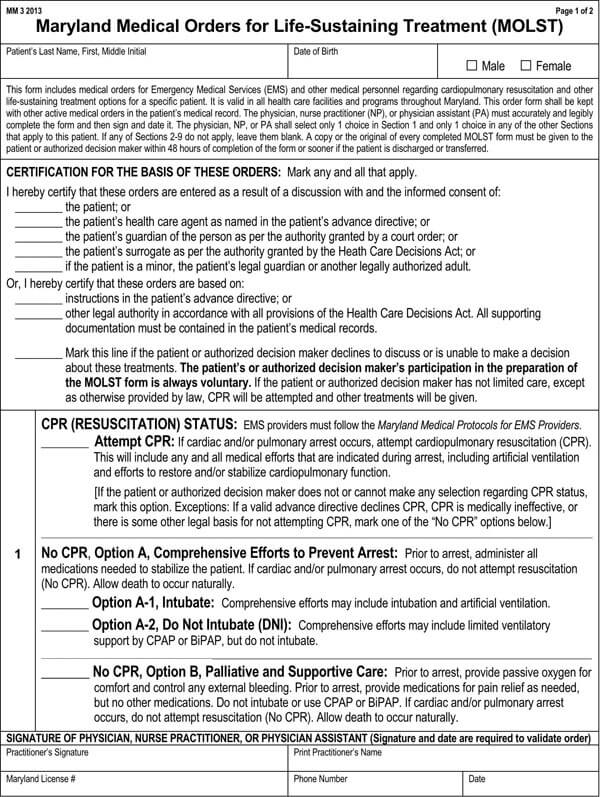
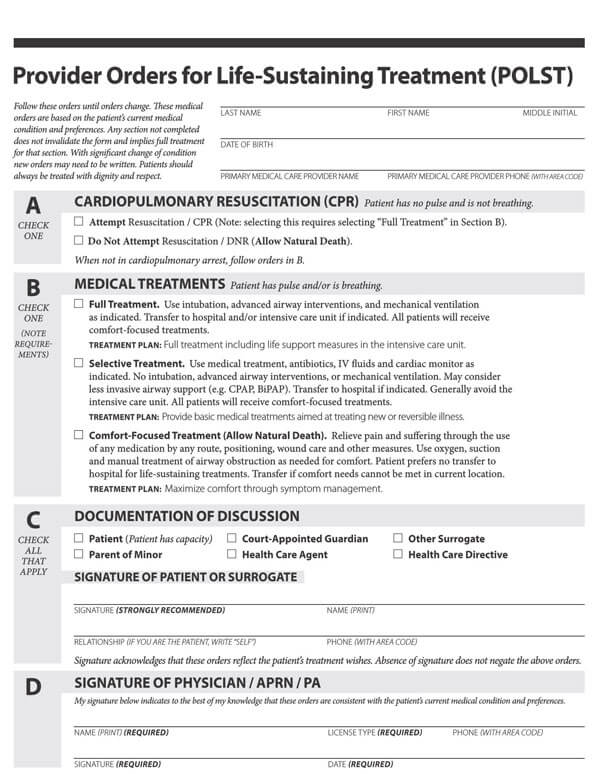
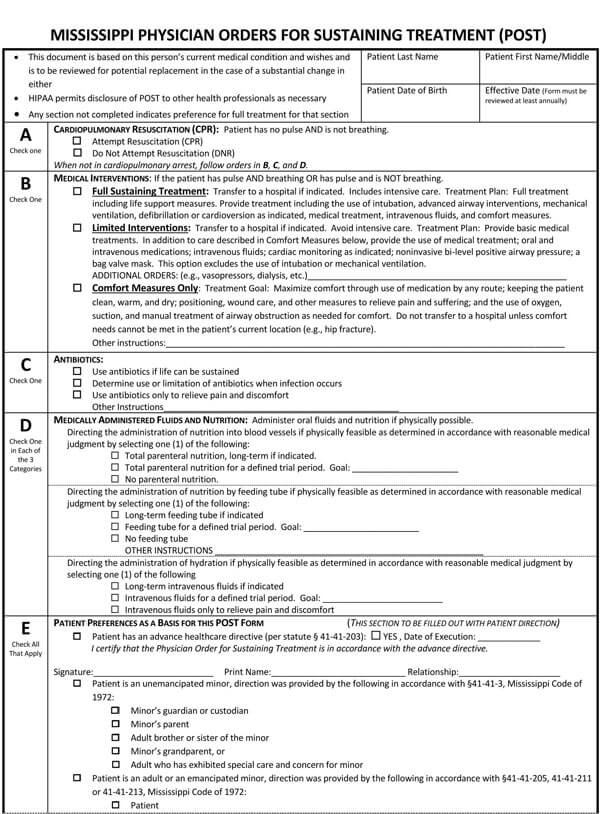
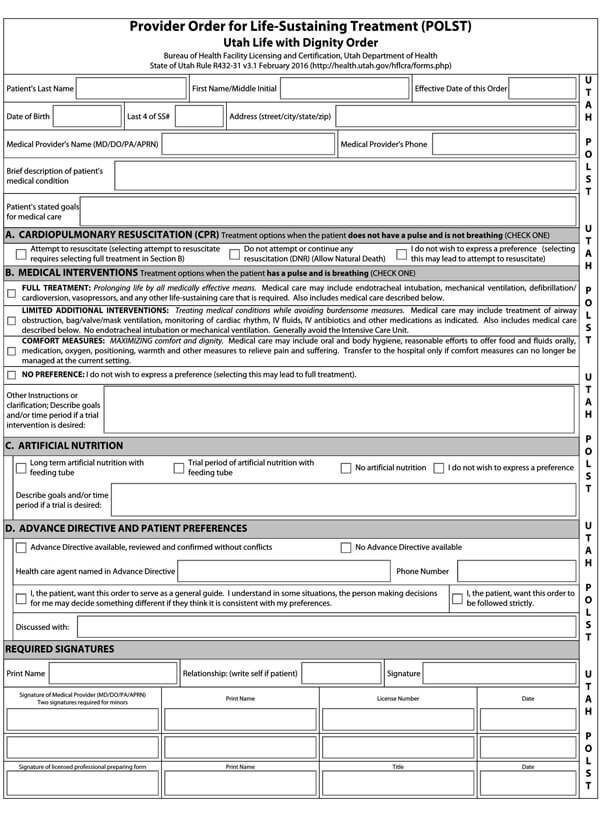
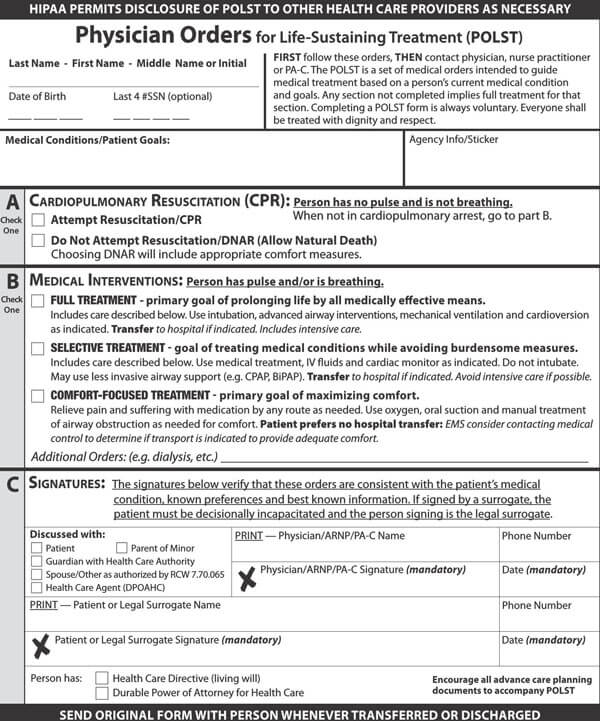
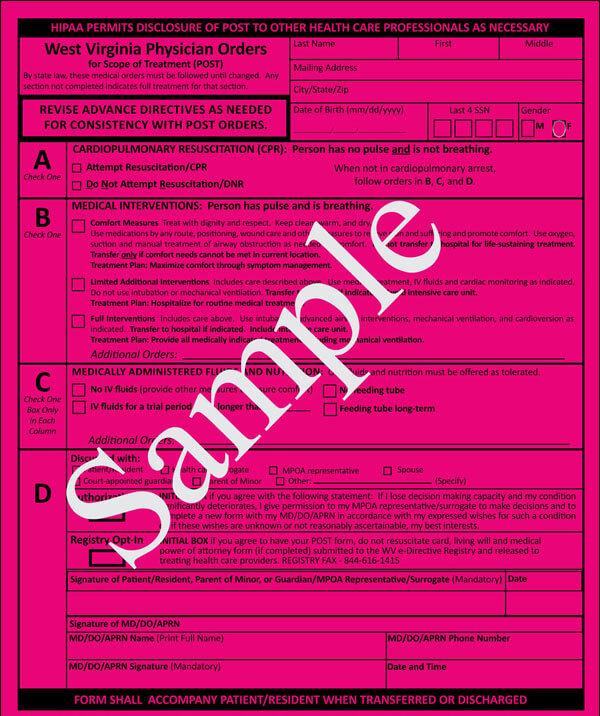
Advance directives may comprise a living will, a Durable Power of Attorney for health care, physician orders for life-sustaining treatment (POLST), or a Do not resuscitate form. All these documents direct and guide your loved ones and doctors about the type of medical care plan you would want if you cannot decide about your health care.
An advance directive may also cover the following end-of-life care and issues;
- Tube feeding/IV feeding– an advance directive may describe how long you’d prefer to be fed through a tube into your stomach or through an IV.
- Ventilation- you can use your Advance Directive to inform your doctor whether you prefer to be ventilated and for how long.
- Palliative care- palliative care is usually all about pain management. You can use the form to describe whether or not you want to receive pain medicine or you prefer dying at home naturally.
- Organ donation- An advance directive should specify if you’d want to donate your organs, tissues for other patients or if you’d donate your body for research.
It is imperative to note that laws about advance directives vary in each state. While Durable Power of Attorney for healthcare and living wills is legal in most states, some states may not recognize them as enforceable laws. Thus, it is important to inquire from your doctor, lawyer, or state representative about your state’s laws regarding Advance directives. But as for DNR orders and POLSTS, they are acceptable in all hospitals and all states.
Types of Patients That Usually Order DNR
Every person has the right to refuse even life-saving medical treatment through advanced care planning methods such as living wills and durable POAs for healthcare. However, not everyone needs a DNR order.
Patients who usually order and obtain DNRs include the following:
The elderly
Extreme measures meant to prolong life, such as CPRs, may negatively impact the quality of life of the elderly. This is because these measures are intended to be used on healthy individuals and not the elderly. Using CPRs on the elderly may lead to brain damage, or they may suffer broken bones, which may undesirably affect their quality of life.
Patients suffering with long term illness
Patients suffering from long-term illness may opt to obtain a DNR from their physician due to the risks involved in CPR procedures. Even if the CPR resuscitates a patient with a long-term illness, it is likely that it will cause more damage to their life, which means that they will no longer breathe without a ventilator’s support.
The terminally ill
Individuals suffering from terminal illnesses such as severe tissue damage by cancer or Alzheimer’s Disease may acquire a DNR order because they do not want to delay the inevitable death. They may opt for a more peaceful or natural death in foreseeable circumstances.
Patients with prolonged pain
Individuals that may have suffered from serious accidents and received severe injuries may obtain DNR orders from their physicians to die a natural death and lessen their pain. This allows the patient’s family to have peace of mind because their patient doesn’t have to suffer anymore.
Dementia patients
Patients ailing from severe dementia may obtain a DNR order so that they can take control over decisions regarding their health care. Individuals suffering from this condition are mentally incapacitated, meaning they are unable to advocate for their right not to be resuscitated in the event of an emergency. However, these individuals are advised to have a form where it is easily visible and accessible to medical personnel.
How to Fill the Do Not Resuscitate Form
Having an Advance Directive of any form, including Do Not Resuscitate orders, is a great idea. It makes a patient’s inclinations about medical care known before they are faced with a difficult situation or illness that renders them uncommunicative. This saves their family and loved ones the hurdle and stress of making difficult decisions about their health care while they are sick. Regardless of your current health status, we all must strive to prepare an advance directive of any sort, such that we are not left out when it comes to decisions regarding our health care.
Various state laws govern the legal requirements regarding DNR forms. Still, DNRs are generally fairly simple to prepare and implement. Regardless, it would be best to be 100% sure that you are following your state’s rules while writing the form.
Typical DNR forms, however, follow these steps:
Obtain the paperwork required to issue a DNR
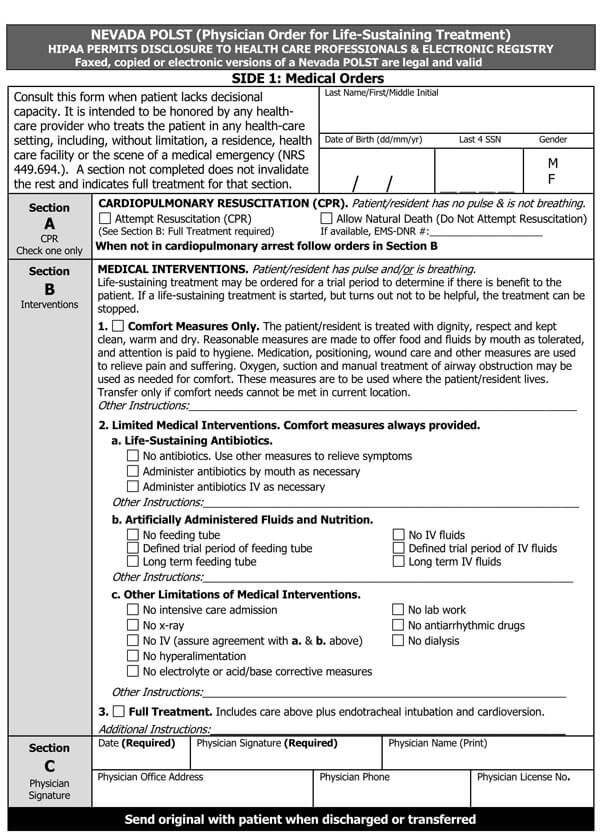
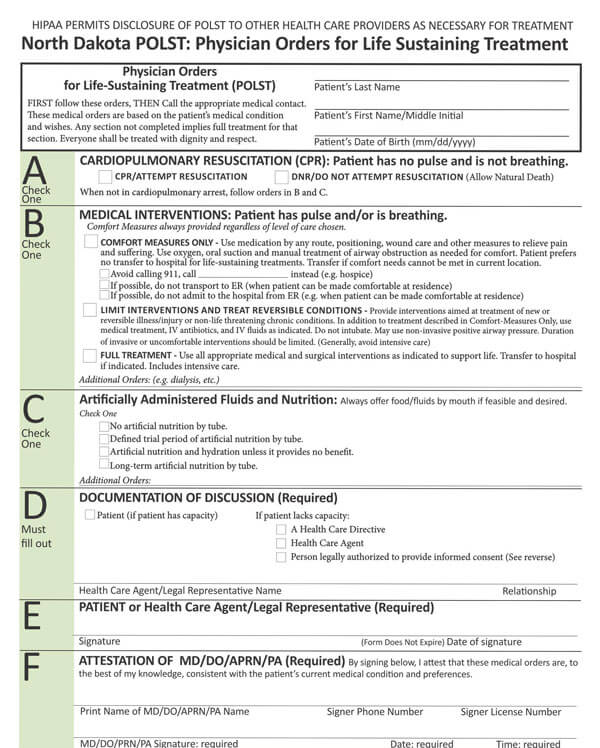
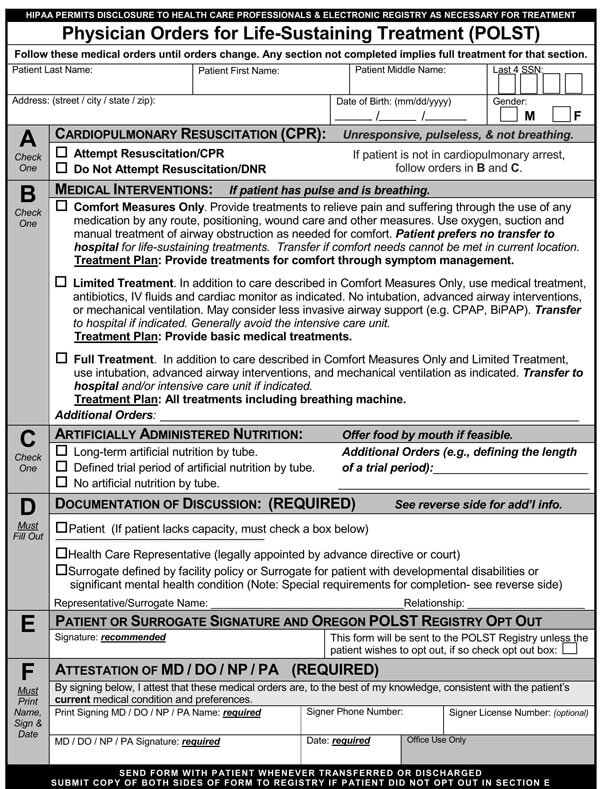
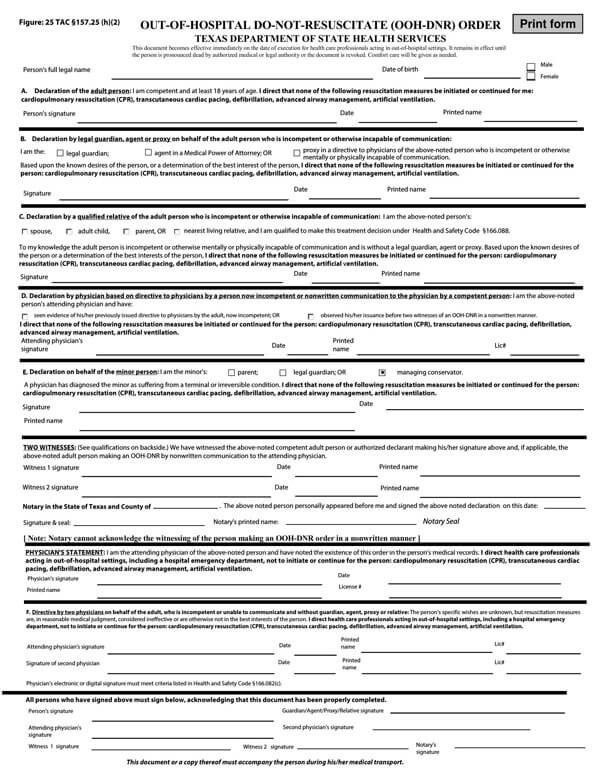
You can download the paperwork from this site using the most compatible format with your computer and printing device. Once you download and fill the document either manually or onscreen, you should have it signed by several parties, including your physician or lawyer, to be taken seriously and legally binding.
Introduction of the patient and their state of residence
After obtaining the required paperwork to issue a DNR, fill in your full and legal name. Your full legal name should come under the subject line that is bolded and capitalized.
Sample:
“DO NOT RESUSCITATE ORDER FOR Mr. Frank Washington.”
After writing the patient’s full legal name, write the state where the patient lives and where this order is governed by law.
Sample:
“This form represents the official request not to resuscitate the patient mentioned above, as is provided by law in the state of Georgia.”
Wishes of the patient
In this segment, the patient must declare their request and make their intention known. The undersigned patient’s name should be presented exactly as it appears on the DNR form title. This should be below the “patient request” section, and the name should precede the term “I.”
Sample:
“I Frank Washington, the undersigned patient, request that resuscitative measures be withheld from me in case of a cardiac arrest or respiratory arrest. I have reached this decision after consulting my doctor, and I am well aware of the consequences of this decision.”
The patient must then sign his/ her name on the signature of the patient section and write the current date on the date section provided in the DNR form. This should be done before witnesses and a notary public who will oversee the whole process.
The status and preferences must be acknowledged and officially supported
The fourth section of the DNR form is the advance directive/living will. This is where the hospital representative admits receipt and understanding of the patient’s directive. This section should be signed by the hospital representative and dated as well. The hospital’s legal name or facility charged with providing care to the patient should also be documented.
For example,
I, Martha Knawels, an authorized representative of XYZ Hospital, hereby certify that the patient named above is significantly incapacitated, therefore, cannot direct his medical care with no hope of regaining that ability. With regard to this statement, I admit to adhering to a duly executed living will with healthcare instructions specifying that no life-sustaining treatments be provided as was beforehand authorized by the patient and as has been documented in the hospital chart.
Similar to the patient request section, this segment must also be signed and dated before a witness and a notary public overseeing the whole session.
A formal declaration with the attorney-in-fact
The patient living directive will usually incorporate a specific person or entity with the power to make decisions regarding the patient’s medical care when he/she is unable to communicate. This party’s participation will be required in this section of the form, “Medical Power of Attorney.” This individual should input their full legal name on the form, followed by their signature and current date of signing the document. The signing of this section should also be done before a witness and a notary public.
Sample:
“I Richard King, the Attorney-in-fact for the undersigned patient as designated by a duly executed Medical Power of Attorney, reserve the right to make decisions about providing, withholding, or withdrawal of extreme life-saving procedures for the patient. With this regard, I hereby direct that life-sustaining treatment be withheld from the patient in the event of a cardiac arrest or cessation of breathing. A copy of this advance directive has been attached herein and has been recorded as part of the patient’s medical record in the hospital chart.”
Declaration of the intent of the health care surrogate
The other party that should participate in the execution of the document is the appointed health care surrogate. In the surrogate consent section, the healthcare surrogate’s name should be entered, followed by their signature and date of signing the official document. The acknowledgment of this statement should be made in the presence of two witnesses and a public notary overseeing the execution.
Physician authorization section
This is where the physician’s statement of official instruction is recorded and the language supplied. This section should be reviewed thoroughly and signed. The physician must declare their full legal names on this section, followed by their signature and date to officially issue the order not to resuscitate and make the document legal.
The verification steps
Immediately all the required sections are filled and signed by the respective parties; the paperwork is surrendered to the witnesses and notary public, who verifies the information presented in the document and signs their names on the witnesses/Notary public section.
As mentioned earlier, you should keep in mind that various states will have different requirements on whom you should use as witnesses and how many are required for this kind of paperwork. Therefore, you should be fully abreast of your state’s requirements before embarking on preparing and issuing the DNR form. Once the required witnesses sign the document, it is handed over to the notary public, who then verifies the signatures of both parties involved, the date, and the location through the notarization process. This is the final step of preparing the DNR form, and it is thus declared a legal and binding document.
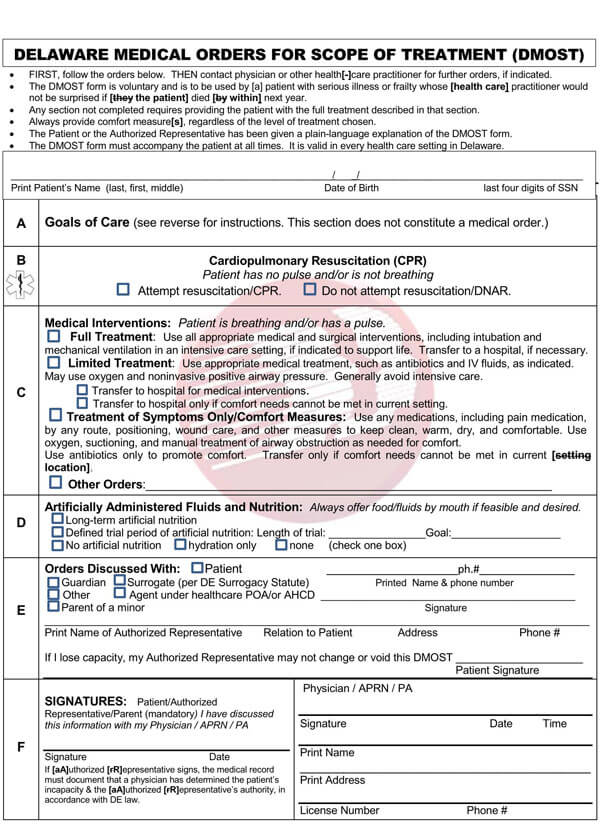
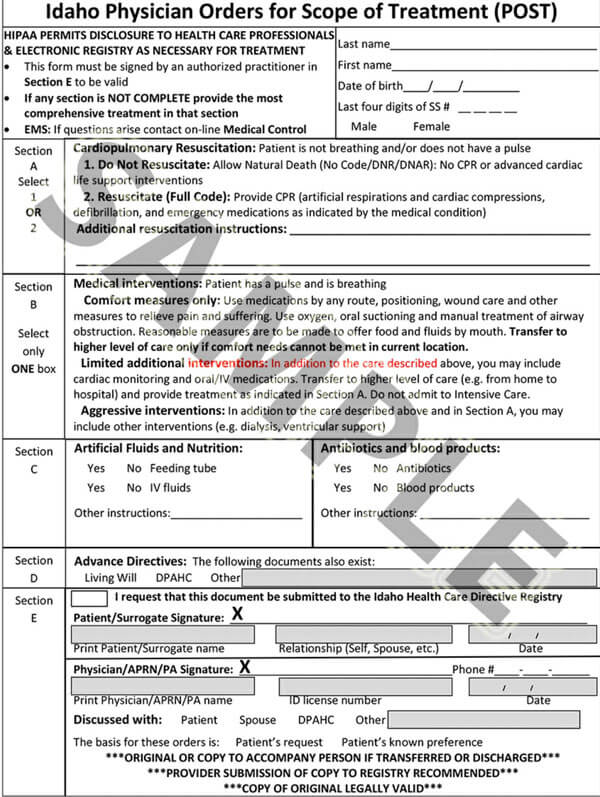
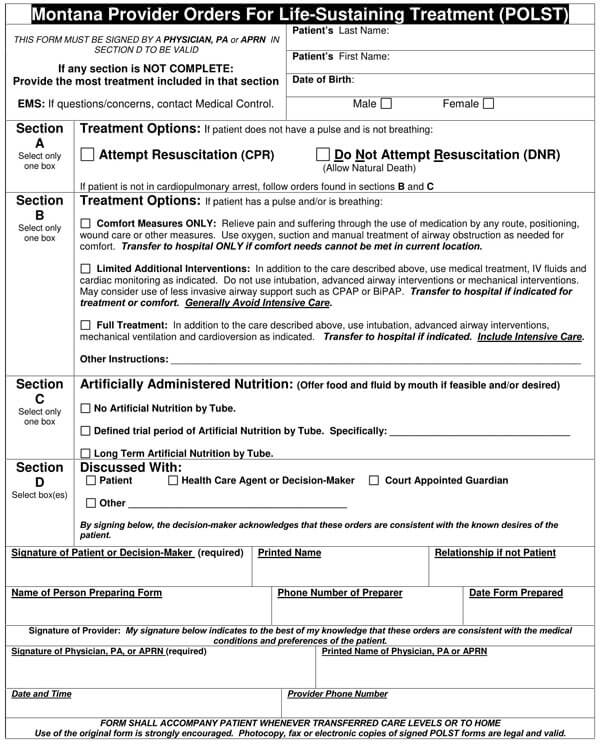
Free DNR Forms & Templates
While modern medicine continues its impressive innovations, you may still find yourself in a wanting situation or a terminal illness that requires you to plan and have an end-of-life treatment and care plan. This is where Do Not Resuscitate Forms come in handy. Though generally easy to prepare, you might need a reference guide. We have provided you with free, premium, and downloadable do not resuscitate form templates that you can use as reference or quickly edit to meet your unique needs. Download our templates today to help you get started.
The 3 Situations that DNR does Not Support
A DNR is not a blanket declaration covering all medical interventions. Instead, it only covers issues relating to cardiopulmonary resuscitation procedures (CPR), intubation via an ET tube, administration of electric shock to patients, and the use of ventilators, etc.
All other forms of treatment, such as providing drugs and chemotherapy for cancer patients, testing, palliative care, pain management procedures, and the various types of supports offered in the modern healthcare provisions, are excluded from the DNR form.
This means that the patient is bound to receive any other treatments unless he/she or their surrogate caregiver states otherwise.
Frequently Asked Questions (FAQS)
I am not sick. Do I need an advance directive?
Contrary to most people’s opinions and assumptions, it is not only the sick that requires an advance directive. Any competent person above the legal age-18 years for most states may opt to have an advance directive for health care. Having an advance directive ensures that you participate in your own healthcare decisions even if you are uncommunicative in the event of an emergency.
What should I include in my advance directive?
An Advance directive includes a living will, Durable Power of Attorney for Healthcare, Physician Orders for Life-Sustaining Treatment, Do Not Resuscitate Orders, Organ and Tissue donation procedures, medical devices to aid in breathing, tube feeding, blood transfusions, dialysis, antibiotics, e.tc. Just make sure that you are precise on the directives to follow and be honored by medical personnel and Emergency responders anytime an accident or illness happens.
Should I pay a lawyer to draft an advance directive on my behalf?
Generally, it is not necessary. However, depending on your state laws regarding advance directives, the DNR form may need to be signed by a witness and a notarized public. It is important that you consult your medical doctor and discuss the impact of your selected end-of-life-treatment care. You can also call your lawyer to review your document to ensure your directives are understood as you intended.
What ensues if I change my mind on the kind of care I want to receive?
It is absolutely okay to reverse your decision about advance directives anytime. All you have to do is destroy the document and all its copies, contact your healthcare provider and your elected surrogate for healthcare and notify them of the same. Still, your changes must be made, signed, and notarized in accordance with your state laws.